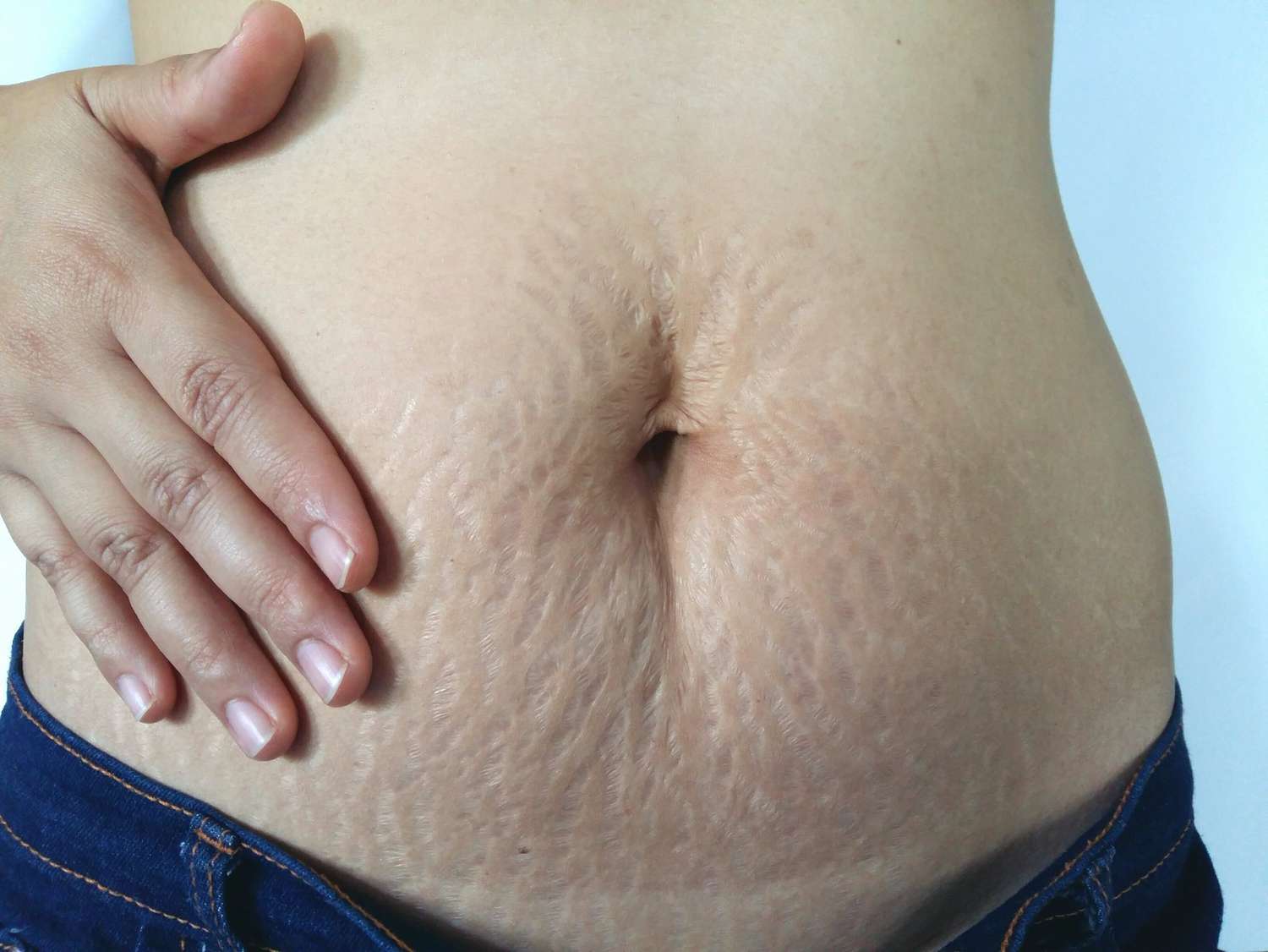
The emotional side of postpartum body changes matters because body changes after birth affect identity, confidence, grief, and the feeling of being at home in your own body. In the postpartum months, mothers are usually not dealing with one single challenge at a time. They are dealing with recovery, sleep disruption, feeding, household demands, emotional changes, and the shock of how much the day now depends on a tiny baby’s needs. Even when a mother expected change, the emotional reality can still feel startling. That is why advice only helps when it fits real homes, real fatigue, and real emotional limits.
A useful place to begin is the most relevant section on New Mother together with the closest related guide. Those pages help connect the immediate problem to a broader postpartum picture. This is not vanity. It is embodiment. In practice, that broader picture is often what helps mothers breathe again: understanding that a hard moment is part of a pattern, not proof of personal failure.
Why this issue feels bigger than it looks
Postpartum and newborn problems often feel bigger than they look because they happen inside deprivation. A tough diaper change at noon is one thing. The same kind of friction at 3 a.m., after physical recovery, interrupted sleep, and five other baby tasks, feels much heavier. That is why so many new mothers feel surprised by the intensity of ordinary moments. A hard feeding loop, a crying window, a body discomfort, or a wave of sadness does not happen in isolation. It happens in a body and household already under strain. That context is what makes the experience feel so total.
What is actually happening in the body or routine
Most of these situations are shaped by a mix of biology, recovery, and environment. Hormonal shifts, healing tissues, sleep fragmentation, baby sleep immaturity, feeding frequency, and the constant start-stop rhythm of newborn care all change how a mother experiences the day. The official guidance at the main evidence-based resource most relevant here is helpful because it grounds that intensity in something real. For emotional health, the NIMH and CDC postpartum materials remind families that mood changes, depression, and anxiety around pregnancy and after birth are common and treatable. For sleep and infant care, the pediatric guidance in AAP/HealthyChildren or CDC resources helps families understand what is developmental rather than personal failure.
Why environment changes everything
Home layout, neighborhood pace, apartment size, family structure, and nearby support all change how postpartum life feels. A narrow hallway, an older building, a high-rise elevator, a multigenerational household, or a tiny bathroom can turn one small task into a repeated friction point. That is why “general advice” often needs translation into the actual place a mother is living. It is also why location-specific stories from Manhattan, Brooklyn, Queens, Jersey City, or West Orange can feel surprisingly validating: the environment is part of the postpartum experience, not just the backdrop.
How mothers commonly misread the situation
New mothers often assume hard means wrong. If the baby is fussy, maybe something serious is being missed. If the body still hurts, maybe healing is failing. If the emotions are mixed, maybe bonding is broken. If nights feel unbearable, maybe everyone else is coping better. Usually the truth is gentler and more complicated. The first step is often not another technique but a better interpretation. This is where the FAQ becomes useful: it helps mothers step back and ask whether what they are feeling fits a common postpartum pattern before they judge themselves for it.
What daily habits usually help the most
The most useful postpartum habits are rarely dramatic. Reduce the number of decisions the evening requires. Create one small station for the task that keeps becoming hard. Eat and drink before you feel wrecked. Keep a short list of grounding actions for hard emotional moments. Use dim light and quiet voices at night. Let one supportive person take one specific part of the routine if possible. If feeding is part of the issue, the guidance at CDC’s formula resource, feeding-item cleaning guidance, and breast milk storage guidance can reduce guesswork. If sleep is part of the problem, CDC safe-sleep guidance and AAP/HealthyChildren safe-sleep guidance help keep solutions both realistic and safe.
When to stop coping alone and reach out
There is a difference between a hard season and a situation that deserves additional support. If sadness or anxiety feels persistent, intense, or frightening; if recovery pain is worsening or seems out of proportion; if the mother is having trouble functioning, bonding, or feeling safe; if feeding or newborn care feels unmanageable rather than merely exhausting, it is appropriate to reach out. The internal path at the contact page is there for exactly that reason, and the support information at CDC, NICHD Moms’ Mental Health Matters, and NIMH reinforces that getting help is part of responsible postpartum care, not a sign of failure.
The practical takeaway
The emotional side of postpartum body changes gets easier when it is placed inside the bigger postpartum reality instead of treated as a standalone flaw in the mother or the baby. Body changes after birth affect identity, confidence, grief, and the feeling of being at home in your own body are usually more manageable once the home, the routine, and the interpretation all become gentler and more realistic. That is what useful postpartum support often looks like: not making everything easy, but making the next hour feel more possible.